Chronic Ankle Instability
What Is Chronic Ankle Instability?
Chronic ankle instability is a condition characterized by a recurring giving way of the ankle joint. This condition often develops after repeated ankle sprains. Usually, the giving way occurs while walking or during sports. Many athletes, as well as others, suffer from chronic ankle instability.
People with chronic ankle instability often complain of:
A repeated turning of the ankle, especially on uneven surfaces or when participating in sports
Persistent (chronic) discomfort and swelling
Pain or tenderness
The ankle feeling wobbly or unstable
A feeling that you don't "trust" the ankle
Anatomy
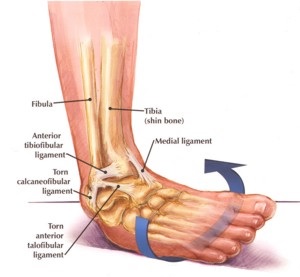
The ankle joint consists of the articulation between the tibia, fibula and dome of the talus. The high degree of congruency confers stability to the ankle but the complex interplay between the surrounding ligaments, as well as the overall alignment of the foot and ankle, is critical to stability. The lateral ligament complex includes the anterior talofibular ligament (ATFL), the calcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL) while medially stability is imparted by the deltoid ligament. When these ligaments become injured and do not heal properly, ankle instability can occur.
Causes
Chronic ankle instability usually develops following an ankle sprain that has not adequately healed or was not rehabilitated completely. When you sprain your ankle, the connective tissues (ligaments) are stretched or torn. The ability to balance is often affected. Proper rehabilitation is needed to strengthen the muscles around the ankle and retrain the tissues within the ankle that affect balance. Failure to do so may result in repeated ankle sprains.
Repeated ankle sprains often cause—and perpetuate—chronic ankle instability. Each subsequent sprain leads to further weakening (or stretching) of the ligaments, resulting in greater instability and the likelihood of developing additional problems in the ankle.
In addition, each ankle sprain can cause damage to surrounding structures such as cartilage and tendons, resulting in permanent disability. This is important, the best time to intervene is early in the process. You do not want your ankle to remain unstable for years. Each minor sprain results in small amounts of damage that in the end can result in catastrophic failure of the ankle and arthritis.
Here is an excellent example of a 55 year old patient that has had chronic ankle instability since a basket ball injury in high school. He did not have it treated and his ankle ultimately ended up deformed and arthritic. He required a total ankle replacement to treat his condition.
Chronically Unstable Ankle
This is an ankle that was unstable for 25 years. This patient is left with a severe deformity and chronic pain due to arthritis. This could have been prevented with an ankle stabilization surgery years prior to reaching this point. If your ankle is unstable, do not wait until it is too late to have it fixed.
Total Ankle Replacement
This is the same patient depicted above. He required a complete replacement of his ankle in order to alleviate his pain and disability.
Diagnosis
Diagnosis is based on a careful history and exam. A history of recurrent sprains and pain are the key to the diagnosis. Physical examination is also important. If the ankle feels unstable on exam or is tender, then this confirms the history. X-rays are important to evaluate for any bony abnormalities, such as fractures of the fibula and damage to the ankle joint.
Stress Views can be done to evaluate the stability of the ankle
Stress views are done in the clinic as well. These are special X-rays performed by the doctor to demonstrate abnormal movement of the ankle. MRI is also an important test to determine if other soft tissues have been damaged, such as the perineal tendons and the cartilage of the ankle.
Nonsurgical Treatment
Treatment for chronic ankle instability is based on the results of the examination and tests, as well as on the patient’s level of activity. Nonsurgical treatment may include:
Physical therapy. Physical therapy involves various treatments and exercises to strengthen the ankle, improve balance and range of motion and retrain your muscles. As you progress through rehabilitation, you may also receive training that relates specifically to your activities or sport.
Bracing. Some patients wear an ankle brace to gain support for the ankle and keep the ankle from turning. Bracing also helps prevent additional ankle sprains.
Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be prescribed to reduce pain and inflammation.
When Is Surgery Needed?
In some cases, surgery is recommended based on the degree of instability or lack of response to nonsurgical treatment. Surgery usually involves repair or reconstruction of the damaged ligament(s). In addition, other structures that are damages will be repaired. Dr. Kemp will order an MRI prior to surgery to assess these structures and tailor your surgical plan to your needs. Dr. Kemp will select the surgical procedure best suited for your case based on the severity of the instability and your activity level. The length of the recovery period will vary, depending on the procedure or procedures performed. But typically your recovery will follow this protocol. Recovery after ankle surgery.
Here is an example of the type of device that may be implanted to help repair your ankle. Dr. Kemp will discuss the best surgery option for you and which implants may or may not be necessary upon request.